In today’s highly digitized healthcare ecosystem, medical coding plays a critical role in bridging clinical care with administrative and financial processes. Every diagnosis made by a physician, every procedure performed in a hospital, and every medical supply used during treatment must be translated into standardized codes. These codes create a universal language that allows healthcare providers, insurance companies, researchers, and government agencies to communicate efficiently. Without accurate coding systems, healthcare documentation would become chaotic, billing processes would be inconsistent, and large-scale health data analysis would be nearly impossible.
Medical coding is essentially the process of converting complex medical information—such as patient diagnoses, treatments, procedures, medications, and equipment—into standardized alphanumeric codes. These codes form the backbone of medical billing and the healthcare revenue cycle. They ensure that healthcare providers receive appropriate reimbursement for the services they deliver while maintaining transparency and compliance with regulatory standards. When documentation is translated into standardized codes, it enables insurance companies to understand the reason for treatment, verify medical necessity, and process claims efficiently. In addition, coding systems play an important role in healthcare research, epidemiology, public health tracking, and hospital performance analysis.
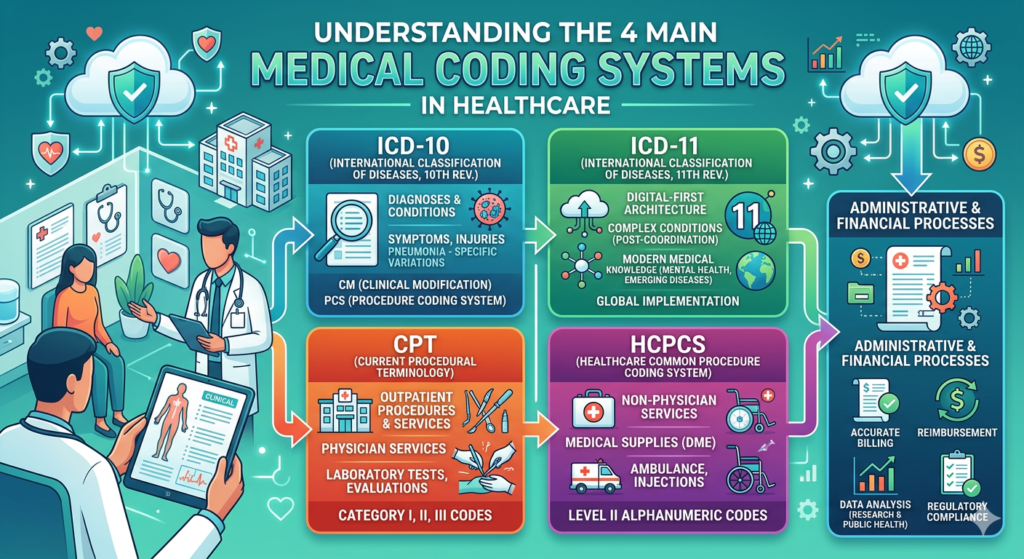
However, medical coding is not always straightforward. The healthcare industry relies on multiple coding systems, each designed to serve a specific purpose. These systems are constantly evolving to accommodate advances in medicine, new treatment procedures, and emerging diseases. For healthcare administrators, medical coders, and billing professionals, understanding the differences between these systems is essential. The four primary medical coding systems widely used in healthcare today are ICD-10, ICD-11, CPT, and HCPCS. Each system contributes uniquely to clinical documentation, billing, and healthcare analytics.
The Importance of Medical Coding in Modern Healthcare
Before exploring the individual coding systems, it is important to understand why medical coding is so essential. Healthcare generates enormous volumes of data every day—from clinical notes and laboratory reports to imaging studies and prescriptions. Without a standardized structure, interpreting this information across hospitals, insurers, and health systems would be extremely difficult.
Medical coding creates that structure. By assigning standardized codes to diagnoses and procedures, healthcare providers can document patient encounters in a way that is universally understood. This standardized language ensures consistency across hospitals, clinics, insurance companies, and public health organizations. It also enables accurate billing because insurance providers rely on these codes to determine reimbursement eligibility.
Another major advantage of medical coding is its contribution to healthcare analytics. Governments and research institutions use coded data to monitor disease trends, identify public health threats, measure treatment outcomes, and allocate healthcare resources effectively. For example, when hospitals consistently code cases of diabetes, cancer, or infectious diseases, policymakers can analyze patterns and plan national healthcare strategies accordingly.
Furthermore, coding accuracy directly affects healthcare revenue cycles. Incorrect codes can lead to claim denials, delayed reimbursements, or compliance penalties. For this reason, medical coders must possess a strong understanding of anatomy, medical terminology, clinical procedures, and coding guidelines. The correct combination of diagnosis codes and procedure codes is essential to justify medical necessity and ensure that healthcare providers receive proper payment for their services.
The Four Core Medical Coding Systems
Although healthcare documentation may appear unified, it actually relies on several specialized coding systems. Each of these systems serves a distinct function within the healthcare ecosystem. Some codes describe diseases and diagnoses, while others focus on procedures, services, equipment, or medications. Understanding how these systems interact is fundamental for healthcare professionals involved in coding, billing, or health information management.
ICD-10: The Global Standard for Diagnoses and Clinical Conditions
The International Classification of Diseases, Tenth Revision (ICD-10) is one of the most widely used medical coding systems in the world. Developed and maintained by the World Health Organization, ICD-10 provides standardized codes for diseases, symptoms, injuries, and health conditions. It allows healthcare professionals to record diagnoses in a structured and internationally recognized format.
ICD-10 replaced the earlier ICD-9 system to improve specificity and expand the number of available codes. The system contains tens of thousands of diagnostic codes, allowing clinicians to capture detailed information about a patient’s condition. These codes use an alphanumeric structure that can describe not only the disease itself but also related factors such as severity, complications, and underlying causes.
For example, a simple diagnosis such as pneumonia may have multiple ICD-10 variations depending on the type of infection, its severity, and associated complications. This level of detail ensures that healthcare providers can accurately document the patient’s condition and justify medical interventions.
ICD-10 is divided into two key components. The first component, ICD-10-CM (Clinical Modification), focuses primarily on coding diagnoses, including diseases, symptoms, and medical conditions encountered during patient care. The second component, ICD-10-PCS (Procedure Coding System), is designed for coding procedures performed in inpatient hospital settings. These procedure codes follow a seven-character structure that describes the type of procedure, the body system involved, the surgical approach, and other procedural details.
The adoption of ICD-10 significantly improved clinical documentation accuracy and enabled better healthcare analytics. By providing more specific diagnostic information, the system supports improved patient care, more accurate reimbursement, and better tracking of disease patterns worldwide.
ICD-11: The Next Generation of Disease Classification
As medical science evolves, classification systems must also adapt. The International Classification of Diseases, Eleventh Revision (ICD-11) represents the most recent advancement in global medical coding. Introduced by the World Health Organization and officially implemented globally in 2022, ICD-11 was designed to address many of the limitations of its predecessor.
One of the most significant improvements in ICD-11 is its digital-first architecture. Unlike previous versions that were adapted from printed manuals, ICD-11 was built specifically for digital environments. The system integrates seamlessly with electronic health records, medical billing software, and data analytics platforms. This digital design improves search functionality, reduces coding errors, and enhances overall workflow efficiency.
Another major advancement in ICD-11 is its modular coding structure. The system allows healthcare professionals to combine multiple codes to describe complex medical conditions with greater precision. This approach, known as “post-coordination,” enables coders to represent conditions in a more detailed and flexible way.
ICD-11 also reflects modern medical knowledge. It incorporates updated classifications for mental health disorders, neurological conditions, infectious diseases, and emerging health challenges. Additionally, it includes new chapters dedicated to areas such as sexual health and traditional medicine, making the system more comprehensive and globally relevant.
Although many healthcare systems still rely heavily on ICD-10, the gradual transition to ICD-11 represents an important step toward modernizing health data management worldwide.
CPT: Coding Medical Procedures and Clinical Services
While ICD codes describe why a patient receives medical care, the Current Procedural Terminology (CPT) system explains what services were performed during treatment. Maintained by the American Medical Association, CPT codes are used to document medical, surgical, and diagnostic procedures performed by healthcare professionals.
CPT codes consist of five numerical digits and are widely used in outpatient and physician billing. They enable healthcare providers to communicate the specific services delivered during a patient visit, such as diagnostic tests, surgical procedures, laboratory analyses, and evaluation or management services.
The CPT system is organized into three categories. Category I codes represent the most commonly performed medical procedures and services. These include areas such as anesthesia, surgery, radiology, pathology, laboratory testing, and evaluation and management services. Category II codes are optional tracking codes used to measure performance and quality metrics in healthcare. They help organizations monitor preventive care initiatives and patient outcomes. Category III codes are temporary codes assigned to emerging technologies, experimental procedures, and innovative treatments that are still being evaluated for widespread adoption.
Because CPT codes directly influence insurance reimbursement, accuracy is essential. If a procedure code does not align with the associated diagnosis code, insurance providers may deny the claim. This makes CPT coding a crucial element of the healthcare revenue cycle and financial sustainability of healthcare organizations.
HCPCS Level II: Coding Medical Supplies, Equipment, and Non-Physician Services
The Healthcare Common Procedure Coding System (HCPCS) complements the CPT coding framework by covering services and items not included in standard CPT codes. HCPCS Level II codes are particularly important for identifying medical equipment, medications, prosthetics, ambulance services, and other healthcare supplies.
HCPCS codes follow an alphanumeric format consisting of a single letter followed by four numbers. The letter prefix groups related items together. For example, certain code ranges represent durable medical equipment, while others represent medications or transportation services.
These codes are widely used in billing processes for government insurance programs such as Medicare and Medicaid. They ensure that healthcare providers can accurately report the use of medical supplies, medications, and specialized equipment provided to patients during treatment.
Beyond billing, HCPCS codes also play a role in healthcare documentation and public health research. By tracking the use of specific medical devices and treatments, healthcare systems can analyze trends in medical technology adoption, patient outcomes, and resource utilization.
The Interconnection Between Medical Coding Systems
Although ICD-10, ICD-11, CPT, and HCPCS serve different functions, they work together to create a comprehensive medical documentation framework. When a patient visits a healthcare provider, the diagnosis is coded using ICD codes to explain the medical condition. The procedures performed during the visit are documented using CPT codes, while any additional supplies, medications, or equipment are recorded using HCPCS codes.
This integrated approach ensures that insurance providers clearly understand both the patient’s condition and the services provided. When codes are accurately linked, claims can be processed efficiently, reducing administrative delays and ensuring proper reimbursement.
The Future of Medical Coding
Medical coding continues to evolve as healthcare technology advances. Artificial intelligence, natural language processing, and automated coding systems are increasingly being used to assist coders in identifying relevant codes from clinical documentation. These technologies have the potential to reduce manual workload, improve accuracy, and enhance revenue cycle efficiency.
However, even with technological advancements, skilled medical coders remain essential. Human expertise is required to interpret clinical documentation, ensure compliance with coding guidelines, and maintain accuracy in complex medical cases.
As healthcare systems continue to expand globally, the demand for professionals trained in medical coding and healthcare management will only increase. Understanding the nuances of coding systems such as ICD-10, ICD-11, CPT, and HCPCS will remain a valuable skill for healthcare administrators, medical coders, and health information specialists.
✅ Conclusion
Medical coding systems form the backbone of healthcare documentation, billing, and analytics. By translating clinical information into standardized codes, these systems enable efficient communication across healthcare providers, insurance companies, and regulatory bodies. The four major coding systems—ICD-10, ICD-11, CPT, and HCPCS—each play a unique role in ensuring accurate diagnosis reporting, procedure documentation, and billing transparency.
As healthcare becomes increasingly data-driven and technology-enabled, the importance of accurate medical coding will continue to grow. For healthcare organizations, investing in skilled coding professionals and modern coding technologies is not just a compliance requirement—it is a strategic necessity for improving patient care, operational efficiency, and financial sustainability.
Medical Coding and the Growing Need for Healthcare Education
As healthcare systems expand and medical technologies advance, the demand for professionals trained in healthcare management and medical documentation continues to increase. Hospitals, healthcare companies, and insurance organizations require skilled professionals who understand both clinical processes and administrative systems such as medical coding.
Institutions like Doctorials Academy are actively contributing to this growing field by providing educational programs and digital learning resources for healthcare students. The academy’s V-Library for MBBS, BDS, and Nursing students provides comprehensive video-based learning resources that help students strengthen their medical knowledge and academic performance.
In addition to clinical learning resources, Doctorials Academy also offers the Post Graduate Diploma in Hospital Management (PGDHM) program. This program is designed to prepare healthcare professionals for leadership roles in hospital administration, healthcare operations, and healthcare management. By combining medical education with healthcare management training, the program helps students build careers in the rapidly growing healthcare industry.


📞 Call / WhatsApp: 9108962129
📩 Email: sh****@***************my.com
Doctors, there is a discount offer
“MBBS, BDS” click here: https://rzp.io/rzp/doctorialsacademyP6wFG9j4
For a limited time
Just for 2500 per year
Website:- https://doctorialsacademy.com/
PGDHM:- https://doctorialsacademy.com/pgdhm/
LinkedIn:- https://in.linkedin.com/company/doctorials-academy
PGDHM LinkedIn: https://www.linkedin.com/company/doctorials-academ-pgdhm/
Abroad LinkedIn: https://www.linkedin.com/company/mbbs-pg-and-pg-abroad-admission/
Facebook:- https://www.facebook.com/people/Doctorials-Academy/61558183675530/
YouTube:- https://www.youtube.com/channel/UCEukyOB7riOSdUhz68tdLzA
Instagram:- https://www.instagram.com/doctorialsacademy/
Android app:- https://play.google.com/store/apps/details?id=com.edmingle.doctorialsacademy&hl=en


